What Is A Knee Arthroscopy?
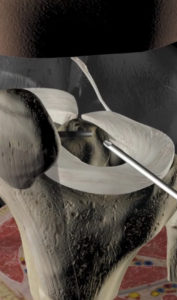
Arthroscopic Knee surgery is a minimally invasive procedure that involves assessment and treatment of damages to the inside of a knee joint.
Knee arthroscopy can be used to treat a number of conditions such as torn meniscus, loose cartilage, damaged cartilage surfaces and anterior cruciate ligament injuries.
What Are The Typical Symptoms?
This will depend on the type of condition you have. Two common conditions Dr Parminder J Singh one of the best knee surgeons in Melbourne will treat include meniscal tears and anterior cruciate ligament rupture.
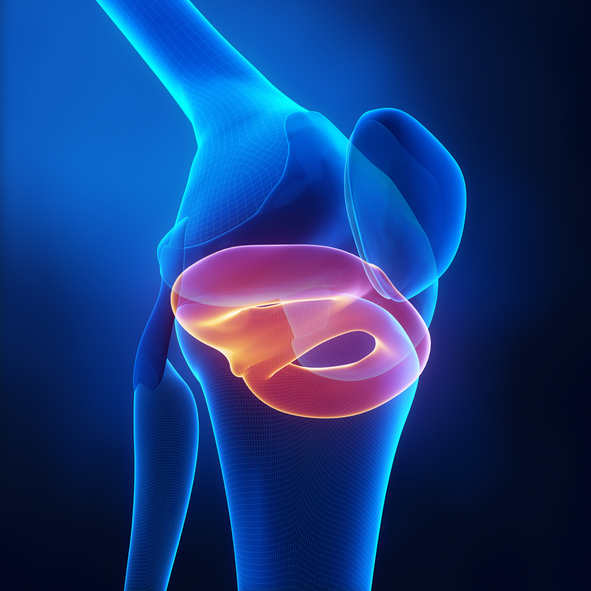
MENISCAL TEARS
Patients will usually present with a history of loading and or twisting their knee. This mechanism of injury can load the meniscus sufficiently to cause a tear. The patient may experience pain around the knee joint line and some mild swelling of the knee. In the presence of very large tears the knee may become locked in position. An MRI scan will help confirm the diagnosis.
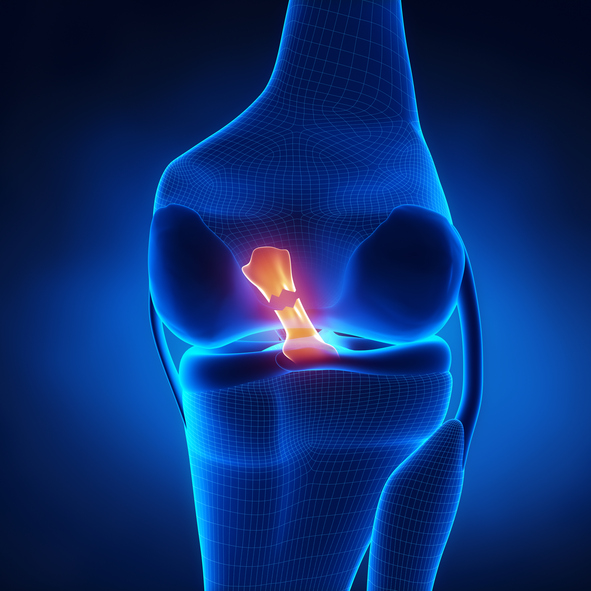
ANTERIOR CRUCIATE LIGAMENT (ACL) INJURY
Patients will usually present with a history of a low-velocity, non-contact, deceleration injuries and contact injuries with a rotational component. Contact sports also may produce injury to the ACL secondary to twisting, valgus (outward angulation of the leg) stress, or hyperextension (bent backwards or overstretched) all directly related to contact or collision. The knee typically swells immediately following the injuries. The knee will be unstable and give way during simple manoeuvres like turning and twisting. Recurrent instability of the knee can lead to further damage to other structures inside the knee joint such as the meniscus, cartilage and bone. An MRI scan will help confirm the diagnosis and also help identify any other structures in the knee that may be damaged such as the meniscus or cartilage
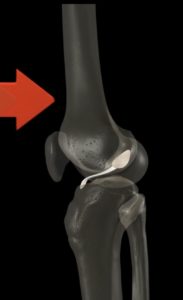
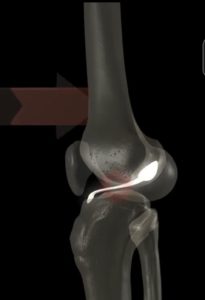
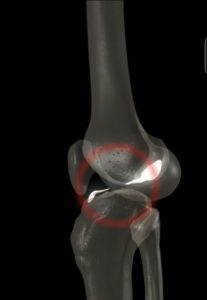
How Is The Surgery Performed?
Patients will usually be admitted as a day surgery procedure and have a general anaesthetic.
MENISCAL TEARS SURGERY
A tourniquet is inflated around your thigh to maintain a bloodless field during the surgery. Typically, two small incisions are made during a knee arthroscopy. One incision for the arthroscope and one for the surgical instruments to treat the knee damage. The keyhole technique usually allows for a more rapid recovery than open techniques as well as shorter recovery times following surgery. The meniscal tear will be either repaired or trimmed depending on the location of the tear in the meniscus. Generally, tears in the zone where there is still a viable blood supply with be repaired and those that are not will be trimmed. Patients are usually able to fully weight bearing after their surgery unless specified by Dr Parminder J Singh.
Dr Singh will see you after your surgery prior to discharge the same day. A follow up appointment will be arranged for you around day 10-14 for removal of stiches. This is performed in rooms and is not usually painful. Rehabilitation may be facilitated with the supervision of a physiotherapist over the period of the next few weeks. Dr Singh will advise you on return to work time and driving based on his clinical assessment following surgery. Patients however would typically be back to work around 1-2 weeks after their surgery, driving after a similar time and normal activities around 4-6 weeks.
ANTERIOR CRUCIATE LIGAMENT (ACL) SURGERY
The ACL is a major stabilising ligament of the knee particularly during movements such as running, twisting and sidestepping.
The function of the ACL is to prevent the femur moving forward and rotating excessively on the tibia. Reconstruction of the ACL will potentially reduce recurrent instability of the knee joint. Usually, patient who are more active and keener to return to sport involving twisting and pivoting will typically proceed to surgery.
Reconstruction of the ACL is performed under a general anaesthetic. A tourniquet is inflated around your thigh to maintain a bloodless field during the surgery. Typically, two or three small incisions are made during a knee arthroscopy. One incision for the arthroscope and the others for the surgical instruments to treat the knee damage. A further 2-3cm incision will be made to harvest your hamstrings.
Your hamstrings will be used to reconstruct the anterior cruciate ligament. Fixation of the ligament will be achieved through a combination of a screw and endo-button. The key hole techniques usually allows for a more rapid recovery than open techniques as well as shorter recovery times following surgery. A check x-ray will be undertaken to endure satisfactory placement of the screw and endo-button prior to your discharge from hospital. An overnight stay is hospital would be typical for ACL reconstruction surgery.
Ice packs used regularly will help with reducing swelling following your surgery. Following your surgery, the physiotherapist will guide you through your rehabilitation. Following your surgery, your ACL graft should be strong enough to put all your weight on the operated leg. You will likely to require crutches and pain killers initially for the first week or two. You may shower providing you have a waterproof dressing over your wounds.
Dr Singh will review your wound approximately 10 days after your surgery and remove any stiches. Patients will need a minimum of 2 weeks of work. Patients who are more active such as labourers may need 2 to 3 months of work. Dr Singh recommends return to competitive sport after 8-12 months following your surgery to reduce the risk of a recurrent injury and it is recommended an experienced physiotherapist helps guide you through your rehabilitation.
What Is The Process Moving Forward?
Step 1: Book A Consultation
If you do require surgery, we will schedule and walk you through the process of your operation.
Step 2 Schedule Surgery
During your appointment, Dr Parminder Singh will take a history, examine you and review the relevant radiology. If any further scans are required Dr Singh will request those. Once the diagnosis has been confirmed Dr Singh will discuss the non-surgical option and surgical options of surgery. If no surgery is required Dr Singh may refer you to a physiotherapist for non-surgical management. If surgery is required Dr Singh will consent you for the surgery explained the risk and benefits of the procedure and the expected outcome.
Step 3 Surgery
Dr Parminder Singh will see you before the surgery in the waiting bay and ensure all your questions have been answered prior to surgery.
Dr Parminder Singh will examine your hip, thigh and leg making sure there are no open wounds or signs of skin infection.
If there are any signs of infection, you surgery will be cancelled and rescheduled for another day. Once this has been check Dr Parminder Singh will draw an arrow on the side of your thigh confirming with you the side of surgery. Dr Parminder Singh will check your consent form to again confirm the operation being performed and side of surgery.
Step 4 Recovery
Following you surgery, you will recover on the ward. Most individual stay one night in hospital and will be seen by the physiotherapist on the ward to facilitate mobilisation using crutches for the first 1-2 weeks.
Some individuals will use the crutches for longer depending on the type of injury and treatment required. Dr Parminder Singh will see you in his rooms approximately 10-14 days after the hip arthroscopy surgery and inspect the hip wound.
The stitches will be removed during this appointment. Dr Parminder Singh will also explain the operative findings and recommended precautions and rehabilitiation required. Another appointment will typically be organised for you around 6-8 week after this date to assesss your progress. In the meantime, rehabilitation is usually recommended with a physiotherapist who has experience with hip arthroscopy patients.
It is important to follow the hip precautions Dr Parminder Singh recommends to allow for the best possible outcome.
Any further appointement will be made on a case by case basis depending your condition. In general terms Dr Parminder Singh recommends approximately 3 months for healing from the surgery and hip precautions during this periods.
Consulting Locations
Richmond VIC 3121
Book a consultation on:
(03) 9428 4128
Brighton VIC 3186
Book a consultation on:
(03) 9428 4128
Boxhill VIC 3128
Book a consultation on:
(03) 9428 4128
343-357 Blackburn Rd,
Mt. Waverley VIC 3149
Book a consultation on:
(03) 9428 4128
Book Online at Waverley Private Hospital
Blackburn VIC 3130
Book a consultation on:
(03) 9428 4128
Book Online at Forest Hill
Gisborne VIC 3437
Book a consultation on:
(03) 9428 4128
Book Online at Gisborne
262 Main St,
Mornington VIC 3931
Book a consultation on:
(03) 9428 4128
Book Online at Mornington
Blanton Dr,
Mulgrave VIC 3170
Book a consultation on:
(03) 9428 4128
108 Bridport Street,
Albert Park VIC 3206
Book a consultation on:
(03) 9428 4128
Book Online at Albert Park
240 Hoppers Lane,
Werribee VIC 3030
Book a consultation on:
(03) 9428 4128
Book a Consultation
Committed to improving the quality of patient advice, treatment and care in the field of orthopaedics, book a one-on-one consultation with Dr Parminder J Singh today.


