 Patient Guide To Total Knee Replacement
Patient Guide To Total Knee Replacement
Written by Dr Parminder J Singh MBBS, MRCS, FRCS (Tr&Oth), MS, FRACS
INTRODUCTION
Osteoarthritis is the most common form of chronic arthritis. The condition affects approximately 1.4 million Australians, or approximately 7.3% of the population. The cause of osteoarthritis (OA) is not completely understood. Being overweight or obese can contribute to OA, particularly in females. Obesity is more strongly associated with OA of the knee than the hip. Individuals with a history of joint trauma or injury are more likely to develop OA. Joint injuries include dislocation, fracture, and tears of the cartilage or ligaments. Congenital abnormalities (conditions that are present at birth) can cause abnormal joint alignment, which may lead to OA. The alignment of a joint affects the load across the cartilage and other tissues. Areas of cartilage under high load or pressure can degrade faster or be damaged by joint movement. This may lead to early-onset OA. OA may run in families. A person is more likely to develop OA if their parents have OA that is early in onset or involves more than one joint
Approximately 97% of total knee replacements performed in Australia are due to OA. The disease is uncommon before the age of 45 years and mostly affects people aged 65 years or over. It is more common in females than in males.
Osteoarthritis usually progresses slowly and may produce non-specific local symptoms that impair health-related quality of life, such as pain with joint use, stiffness, loss of joint mobility and function and alteration in the shape of the joint. The knee is most commonly involved, followed by the hip. The spine, foot and joints of the hand can also be affected.
The knee is the largest joint in your body. In a normal, healthy knee, the bone surfaces that come together at the joint are smooth and hard. A cushioning layer of tissue (called articular cartilage) prevents contact among these bones. This tough layer of tissue allows the bones to move without creating friction or wear on the bone surfaces. As the cartilage breaks down, the underlying bone is often left exposed and unprotected, producing bony spurs called osteophytes. In addition, soft tissues around the joint (such as the synovium, ligaments and tendons) can become inflamed and swollen. As these changes occur, the joint loses its smooth movement, becoming stiff and painful. Reduced use of the painful joint causes the muscles to weaken and lose bulk. This in turn increases the load and damage to the cartilage, bone and soft tissues. In advanced stages of OA, the space between the bones is reduced and bones can be in direct contact during movement. This results in increased pain and further joint damage.
 Early Non Operative Treatment Of Knee Arthritis
Early Non Operative Treatment Of Knee Arthritis
Initially, medication and walking aids and physiotherapy may help with the symptoms temporarily.
Medications commonly prescribed for OA include paracetamol, paracetamol combinations and non-steroidal anti-inflammatory drugs (NSAIDs). Paracetamol acts to reduce pain, whereas NSAIDs reduce both swelling and pain. Glucosamine and chondroitin are two of the most common supplements taken for OA. These are derivatives of cartilage components known as glycosaminoglycans.
Physical therapy and exercise can strengthen the muscles surrounding the joints and improve cartilage nutrition and health.
Mechanical aids such as walking sticks, orthotics and bracing can also protect the joints from further damage.
Weight loss from exercise and controlled dieting can reduce the severity of symptoms in people with knee OA. Weight loss reduces the impact load on the joint and may reduce pain.
If other treatment options no longer provide sufficient relief, a total knee replacement is cost-effective and highly successful surgical procedure for the majority of people. A successful joint replacement should help relieve pain, deformity and disability.
 Prior To Surgery
Prior To Surgery
Prior to surgery, to reduce the risk of infection or wound healing problems, smoking should be stopped at least one week prior to surgery. Dr Singh will organise a dedicated physician, anaesthetist and to review your medical history and provide you with all the preoperative instructions you need including fasting times. Stopping eating and drinking at least 6 hours prior to your surgery will reduce the risk of vomiting whiles you are under anaesthesia.
If you are taking any medication, you will receive instructions about safe doses to take in the days leading up to surgery. In particular stop taking any anti-inflammatory medicine at least one week prior to surgery, to prevent excessive bleeding during the surgical procedure.
 Surgical Procedure
Surgical Procedure
Total knee replacement surgery was first performed in 1968. Since then, knee replacement surgeons have been using improvements in surgical materials and techniques have greatly increased its effectiveness. Total knee replacement, or total knee arthroplasty, is a surgical procedure in which parts of the knee joint are replaced with artificial parts (prostheses). Dr Singh has been performing knee replacement surgery since 2004.
The type anaesthesia include epidural, spinal, or general, and will be decided upon by your surgeon and anaesthetist, who will review with you the advantages and disadvantages.
The operation takes place with an anaesthetic, antibiotic cover and usually a tourniquet around the thigh to reduce the amount of bleeding particularly at the time of fixation of the implants. Dr Singh and his team wash and prepares the leg with an antibacterial solution and will wear protective clothing at the time of surgery in the form of a Charnley exhaust suit, disposable gown plus visor and the Steri-Shield system.
Prior to your total knee replacement, Dr Singh will plan which technology to use in order to optimize the surgery. There is a constant emergence of new technology including robotic assisted surgery, patient match cutting blocks that Dr Singh will consider in planning the best way to perform the surgery.
During a total knee replacement operation, Dr Singh will remove the damaged surfaces. The replacement surfaces will then be fixed into place. The surface of the upper bone (femur) is replaced with a rounded metal component that comes very close to matching the curve of your natural bone. The surface of the lower bone (tibia) is replaced with a flat metal component and a thin flat-shaped polyethylene plastic to serve as the cartilage. The underside of the kneecap (patella) may be replaced with a polyethylene plastic component.
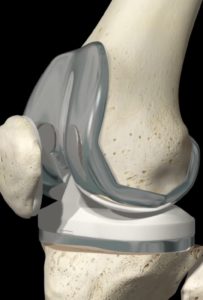
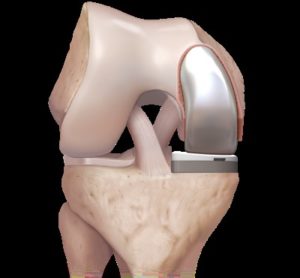


The incision is typically placed midline over the knee joint and can be approximately 10 to 15cm in length depending on the size of the leg. The blood vessels, muscles and nerves are protected during surgery and special tools are used to measure and remove the damaged surface of the bone. When necessary, Dr Singh may use individualised patient cutting blocks to help reshape the knee to optimised the component placement. The components may be implanted by shaping the bone to form a tight fit with the prosthesis, bone cement may be used to hold the prosthesis in place (cemented).
During the operation, Dr Singh will check the alignment of the knee as well as test function and stability of the knee joint.
A special pain catheter will be placed onto the knee joint to facilitate post-operative pain control for 24 hours after your surgery. With this type of pain control technique your morphine requirement should be less and therefore less post-operative nausea and vomiting and constipation and facilitate early mobilisation. Often Dr Singh will encourage early mobilisation on day one after your surgery if your pain is particularly well controlled. The wound is closed with internal stitches to keep all the ligaments and muscles securely together, and sutures or special tape on the skin.
Unfortunately, if the replacement becomes loose, or gets infected another operation is necessary; this is called a revision knee replacement in order to replace the old replacement with a new one.
Following the total knee replacement you will be transferred from the operating theatre into the recovery area where there may be several other patients. You will be here for up to 1-2 hours while most of the anaesthetic wears off. If you have had a spinal anaesthetic you may not be able to feel your legs initially when you wake up.
 In The Hospital – Knee Replacement Recovery Time
In The Hospital – Knee Replacement Recovery Time
The day after your surgery, it is also important to get out of bed and mobilise (initially under supervision by the physiotherapist and nursing staff) to reduce digestive/circulatory problems and encourage healing. Delay in mobilisation can increase the chances of developing post operative constipation and clots in the leg.
Both Dr Singh and your physiotherapist will be on hand to give specific advice on pain control, wound care, diet, exercise and how much weight you can put on your operated leg (weight bearing). If the knee is particular stiff following surgery, Dr Singh may order a machine to help begin to move your knee up and down.
During your stay, a physiotherapist will visit you on the day after your surgery and teach you how to use your new knee. It is important that you get up and about as soon as possible after surgery. Even when lying in bed you can “pedal” your feet on a regular basis in order to promote blood flow in your legs. It is during your stay in hospital that your physiotherapist will help you to achieve the activities such as getting in and out of bed, walking and going up and down stairs. Also moving about (using a frame or crutches), and using the toilet. The physiotherapist will guide you through performing every day activities such as bathing, range of motion and strengthening of your knee.
While in the hospital, Dr Singh recommends you wear tight-fitting, anti-embolism stockings that help control swelling in your legs. They are allowed to be removed daily for bathing and then should be reapplied. The stockings should be worn day and night for up to six weeks after surgery.
You will be ready to leave the hospital when you can get in and out of bed and a chair, go up and down a few stairs, bend your knee between 80 and 90 degrees, and manage your pain with oral medication.
You should be able to fully bear weight on your leg when discharged from the hospital, but most patients may need to use crutches, a cane, or a walker for a few weeks until they are comfortable walking on their new knee. You will be given a prescription for pain medication and schedule a series of follow-up visits starting sometime around six weeks after surgery.
 Discharge From Hospital To Home
Discharge From Hospital To Home
Depending on how well you heal after the surgery, your stay in hospital can vary from between 4 to 10 days and you will need help at home for several weeks. Based on your own individual circumstances you will be able to go directly home or a rehabilitation centre after your surgery. Any sutures that need to be trimmed or removed is usually done around 10 to 14 days following your joint replacement.
Dr Singh recommends that you follow your physiotherapy program and generally avoid strenuous activities that may irritate your knee typically for first six weeks following surgery. The goal is to restore your motion and improve your strength. Progressively walking longer distances each day is helpful.
Try to arrange for someone to visit you at home to help you for up to six weeks. You may need assistance with putting on the elastic stockings, cooking, doing laundry, cleaning, and getting around town. Whenever possible during the first few weeks after surgery, you should periodically elevate your leg to help reduce the swelling. It is normal to have swelling for the first 3 to 6 months after surgery.
Most patients may shower when they get home. Dr Singh recommends your wear a waterproof dressing and avoid bathing for 6 weeks
Following your surgery, you may feel pain or discomfort for the first few weeks at home and you should make sure your prescribed pain control medication as required. Taking one every four to six hours as directed is usually required for the first few days to suppress pain.
Swelling in your knee usually slowly reduces over the first few weeks following surgery. The surgical incision should be dry, but there may be occasional slight spotty bleeding along the wound. A light dressing may cover the incision and the compression stockings should be worn at all times for the first six weeks. Icing your knee for 20 to 30 minutes a few times a day during the first few weeks after surgery will help reduce pain and swelling. If you notice increased swelling, redness, or wound bleeding, you should call Dr Singh’s team.
The presence of new onset calf pain, chest pain or shortness of breath can be a sign of a possible blood clot. Please arrange see your doctor immediately if you notice any of these symptoms
 TIPS FOR YOUR KNEE
TIPS FOR YOUR KNEE
- Following your surgery, you may feel pain or discomfort for the first few weeks at home and you should make sure your prescribed pain control medication as required. Taking one every four to six hours as directed is usually required for the first few days to suppress pain.
- Swelling in your knee usually slowly reduces over the first few weeks following surgery. The surgical incision should be dry, but there may be occasional slight spotty bleeding along the wound. A light dressing may cover the incision and the compression stockings should be worn at all times for the first six weeks. Icing your knee for 20 to 30 minutes a few times a day during the first few weeks after surgery will help reduce pain and swelling. If you notice increased swelling, redness, or wound bleeding, you should call Dr Singh’s team.
- The presence of new onset calf pain, chest pain or shortness of breath can be a sign of a possible blood clot. Please arrange see your doctor immediately if you notice any of these symptoms
- Dr Singh recommends that you follow your physiotherapy program and generally avoid strenuous activities that may irritate your knee typically for first six weeks following surgery. The goal is to restore your motion and improve your strength. Progressively walking longer distances each day is helpful.
- Try to arrange for someone to visit you at home to help you for up to six weeks. You may need assistance with putting on the elastic stockings, cooking, doing laundry, cleaning, and getting around town. Whenever possible during the first few weeks after surgery, you should periodically elevate your leg to help reduce the swelling. It is normal to have swelling for the first 3 to 6 months after surgery.
- Most patients may shower when they get home. Dr Singh recommends your wear a waterproof dressing and avoid bathing for 6 weeks
 TIPS FOR HOME
TIPS FOR HOME
- The following tips can be useful in making your return home more comfortable. Consider placing items that are used regularly at your hand height. Try to avoid very high or very low shelves as these may require the use of steps or kneeling.
- Your furniture should be positioned so that you can manoeuvre with easily and safely with a frame or crutches and reduce the risk of a fall. Remove rugs and place non-slip mats in your bath. It may even be worth changing rooms around by placing a bed downstairs to reduce the use of stairs for the first few weeks.
- With respect to transport, you may sit in a car but only if you follow Dr Singh’s and your physiotherapist instructions for entering and exiting the vehicle. You may need to raise your car seat with pillows to protect your hips and knees. Dr Singh will inform you when you can drive which will typically around six weeks after surgery. Please ensure you can perform an emergency brake, without discomfort, before attempting to drive.
- Ideally make sure you have a good chair with arms that is both firmer and higher than a normal low seated chair as these are safer and more comfortable. However it should not be so high that your legs dangle or lead to pressure on the back of the thigh.
- Installing a gripping bar and a non-slip mat in the shower is sensible; and a raised lavatory seat may be added if required. My Singh’s pre-assessment nurse will be able to provide some further information on where to hire this equipment and which may be best suited for you.
- To assist in certain manoeuvres following your surgery, consider the use a long handled shoe horn, long handled bath sponge or a grabbing tool to avoid bending over too far may be helpful. Initially, you may need someone to assist you putting on your socks and tying your shoelaces. Use long handled feather dusters or low and high items. Do not sweep, mop or vacuum until Dr Singh tells you it is safe to do so.
 MEDICATION
MEDICATION
Dr Singh will prescribe blood thinning medication to reduce your risk of forming blood clots for a period of 6 weeks. Anti-Embolism precautions, including regular exercise should continue for 6 weeks.
Be sure to notify your dentist you have had a recent knee replacement and let your surgeon know if your dentist schedules an extraction, periodontal work, dental implant or root canal work. It may be necessary to take an antibiotic to reduce the risk of infection of the joint replacement.
 SITTING
SITTING
Dr Singh recommends that at least the first 3 months, sit on chairs that have arms. Using low chairs, low stools, or reclining chairs may be more difficult initially. The physiotherapist will show you how to get in and out of a chair keeping your operated leg out in front of you. Crossing your legs and kneeling is not recommended following your surgery.
 ASCENDING AND DESCENDING STAIRS
ASCENDING AND DESCENDING STAIRS
If you are going up stairs, put your un-operated leg on the step above and then lift your operated leg followed by the crutches. If you are going downstairs, put your crutches first, then your operated leg and finally followed by the un-operated leg.
 DRIVING
DRIVING
As a guideline, you should begin to drive at 6 weeks and Dr Singh will be able to confirm this for you depending upon you individual circumstances.
 GETTING IN AND OUT OF YOUR CAR
GETTING IN AND OUT OF YOUR CAR
Move the seat back as far as possible and make sure you get into the car bottom first. Gradually lower yourself, keeping the operated leg a little further out. Gently slide back onto the seat as far as possible before swinging your legs into the car. In order to get out of the car, repeat the process in reverse. You may consider the use of a sheet of polyethylene to facilitate with sliding and turning on the seat.
 WALKING
WALKING
Most patients will attempt their first few steps on day one following surgery with a frame and supervision with the physiotherapist. First move the walking aid forward, then step with your operated leg and then move your un-operated leg. As your walking improves the physiotherapist will progress you to walking with crutches followed by a stick which may be used for up to six weeks after your surgery. During the first few weeks, your aim rehabilitation will be to stretch and strengthen your muscles around the knee and restore your range of motion. As your strength improves, the range of motion should also improve. You may take up to six weeks off from work, depending on the type of job you perform. Following your total knee replacement, Dr Singh strongly advises against doing activities that produce high impact loads such as running and jumping. Sports such as golf, cycling, swimming, and walking are fine.
 RETURN TO WORK
RETURN TO WORK
The duration of time it takes for you to return to work depends on the type of activities you perform. Generally this time can be approximately 6 weeks. Dr Singh will be able to advise you based on your individual circumstances.
 OTHER ACTIVITIES
OTHER ACTIVITIES
Total knee replacement is a predictable and durable procedure in the majority. How you treat your new knee will influence its longevity. Therefore, it is important to know which activities are permissible and which are not following total knee replacement. As soon as the stitches have been removed and the wound is dry you can begin swimming provided appropriate aids are present, (pools with step ladders to get in and out are not recommended and avoid twisting movements to begin with). Initially, avoid activities that place stress on the joint such as lawn bowls, tennis, badminton, horse riding, any contact sports or jogging until discussed with Dr Singh at your follow up appointment. Do not do any heavy lifting initially. Your Physiotherapist will also help guide you through activities to do and avoid following your joint replacement. These precautions are necessary to prevent the new knee from dislocating and reduce the risk of complications. Don’t cross your legs for at least 8 weeks and avoid turning your feet excessively inward or outward. Remember not to use pain as a guide for what you can and cannot do.
For sports and fitness regimens must be individualized. Participation in sports and recreational activities should be discussed with your surgeon and physiotherapist.
Recommended Activities following your total knee replacement Gentle Cycling, swimming, low-resistance rowing, stationary skiing machines, walking, hiking, and low-resistance weight lifting all are excellent ways to maintain fitness without overstressing the implant.
Activities to avoid following your total knee replacement generally, high-impact activities that cause high stress loads on the implant and therefore may potentially increase the risk of early failure. Specific activities to avoid include baseball, basketball, football, hockey, soccer, basketball, high-impact aerobics, gymnastics, jogging, power lifting, rock climbing, hang gliding, and parachuting.
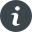 GENERAL GUIDE TO PHYSIOTHERAPY
GENERAL GUIDE TO PHYSIOTHERAPY
Dr Singh and your physiotherapist will guide you through your rehabilitation following your knee replacement. Physiotherapy forms an important part of your recovery and can have a significant influence on the speed of your recovery and the muscle control you have over your new knee. Your physiotherapist will give you your own set of exercises to perform. The exercises listed below are a general guide to movements you can perform both before and after your knee replacement. The rationale for doing the exercises prior to your operation is that you will build up the muscles around your knee and make the exercises afterwards easier. Generally, try to perform your exercises 2 – 3 times daily with 10 repetitions each time. Initially you may find them difficult, so aim to increase movement with gentle repetition. As you progress try to hold each exercise for around 5 seconds. Remember, to perform your exercises safely.
A) Lie on your back or sit with your legs straight, pull your feet up towards you and push your knees down firmly against the floor/bed. Hold for 5 seconds then relax. This exercise can be combined with a knee bent as below.
B) Place a rolled blanket under your knee. Pull your feet towards you and tighten your thigh muscles to straighten the knee (keeping the back of the knee on the roll). Hold for 5 seconds.
C) Pull your toes up; straighten the knee and lift the leg 20 cm off the floor/bed. Hold for approximately 5 second then slowly relax.
D) Lay or sit with a sliding board under your leg. Bend and straighten your knee by sliding your foot up and down the board.
E) Sit on a high chair or table. Bend your knee underneath as much as you are able comfortably. Hold for 5 seconds.
F) Sit on a chair with a cushion under your thighs. Pull your toes up, tighten the front of your thigh muscle and straighten your knee slowly. Hold for approximately 5 seconds.
G) Stand, holding onto a support. Bend your knee and lift your foot off the floor to approximately 45 degrees. Hold for approximately 5 seconds.
H) Holding onto a support, push up with your toes.
I) Holding onto a support, place your affected foot onto a step; slowly shift your weight forward over that foot, allowing your knee to bend as much as possible maintaining a stable position.
J) Stand in front of a small step. Step up with your affected leg on the step. Initially after your surgery, you will need a cane in the opposite hand to the operated leg to help provide some additional support.
K) Stand up and then sit down slowly on a chair (This can be made easier and more difficult by changing the height of the chair). Initially, try to use a high seated chair and avoid the low seated chair.
L) Holding onto a support, stand on one leg Push up on your toes.
M) Standing with support available. Squeeze a foam wedge/towel between your knees, continue to squeeze while gently bending your knees to 45 degrees. Return to standing and relax.
N) Leaning with your back, against a wall and your feet about 20 cm from the wall, slowly slide down the wall, until your hips and knees are at right angles. Try to hold for 15 seconds. Return to starting position.
O) Stand on the operated leg. Try to balance, without holding on for 60 seconds.
 Parminder J Singh Publications On Total Knee Replacement
Parminder J Singh Publications On Total Knee Replacement
Singh PJ, Kotnis R, Bulstrode C. Expert Review – Clinical Examination of the Knee Joint. The Journal of Clinical Examination, Feb, 2007 http://www.bjjprocs.boneandjoint.org.uk/content/93-B/SUPP_II/94.2.abstract
Caroline Blackey, Yogesh Kamat, Parminder Singh, Alexander Dinneen, Anne Vie, Vipul Patel, Ajeya Adhikari, Richard Field. The Oxford Knee Scores for Primary Total Knee Replacement. J Bone Joint Surg Br,2011 Vol. 93-B no. SUPP II 94
Abstract
Publication of normal and expected outcome scores is necessary to provide a benchmark for auditing purposes following arthroplasty surgery. We have used the Oxford knee score to monitor the progress of knee replacements undertaken since 1995, the start of our review programme.4847 Oxford assessments were analysed over an 8 year follow-up period.
The mean pre-operative Oxford knee score was 39.2, all post-operative reviews showed a significant improvement. Patients with a BMI > 40, and the under 50 age group showed early deterioration in outcome scores, returning to pre-operative levels by 5 and 7 years respectively.There was no significant difference in outcome between surgeons performing < 20 knee replacements a year and those performing > 100 / year.
The age of the patient at the time of surgery and the pre-operative body habitus have been identified as factors affecting long term outcome of total knee replacement surgery. Awareness of these factors may assist surgeons in advising patients of their expected outcomes following surgery.
International Presentations
Kamat Yogesh, Singh Parminder, Dinneen Alexander, Vie Anne, Patel Vipul, Adhikari Ajeya, Field Richard. The Oxford knee scores for primary total knee replacement. Efort June 2-5th 2010, Madrid, Spain.
For further information on arthritis go to:
http://www.arthritisvic.org.au/
Arthritis Victoria, 263-265 Kooyong Rd, Elsternwick, Vic, 3185 Freecall 1800 011 041
Consulting Locations
Richmond VIC 3121
Book a consultation on:
(03) 9428 4128
Brighton VIC 3186
Book a consultation on:
(03) 9428 4128
Boxhill VIC 3128
Book a consultation on:
(03) 9428 4128
343-357 Blackburn Rd,
Mt. Waverley VIC 3149
Book a consultation on:
(03) 9428 4128
Book Online at Waverley Private Hospital
Blackburn VIC 3130
Book a consultation on:
(03) 9428 4128
Book Online at Forest Hill
Gisborne VIC 3437
Book a consultation on:
(03) 9428 4128
Book Online at Gisborne
262 Main St,
Mornington VIC 3931
Book a consultation on:
(03) 9428 4128
Book Online at Mornington
Blanton Dr,
Mulgrave VIC 3170
Book a consultation on:
(03) 9428 4128
108 Bridport Street,
Albert Park VIC 3206
Book a consultation on:
(03) 9428 4128
Book Online at Albert Park
240 Hoppers Lane,
Werribee VIC 3030
Book a consultation on:
(03) 9428 4128
Book a Consultation
Committed to improving the quality of patient advice, treatment and care in the field of orthopaedics, book a one-on-one consultation with Dr Parminder J Singh today.





